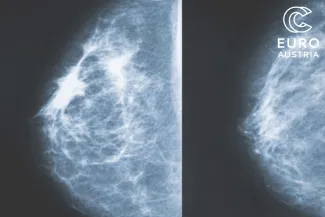
With support from EuroCC Austria, Austrian start-up Salataris AI developed a deep learning model that supports medical experts in identifying tumours at an early stage. The model was trained on mammography and MRI images to detect even small and rare tumours.
Breast cancer is the most common form of cancer among women – and although men are affected far less frequently (around one percent of cases), they are not exempt. In Europe, approximately 660,000 people are diagnosed with a malignant breast tumour each year – about the same as the population of Luxembourg. Every year, 156,000 people die from the disease – roughly equivalent to the population of Heidelberg, Germany. All this is caused by just a few rogue cells. If they could be detected earlier and more accurately, thousands of lives could be saved.
The challenge: better image data is needed
This is exactly where Salataris AI aims to contribute: supported by EuroCC Austria, the team is developing an AI model to detect breast cancer in mammography and MRI (magnetic resonance imaging) scans. The first step is to improve the image data. Mammography and MRI images often contain so-called artefacts – distortions in the image, such as speckled patterns or fine-grained noise, which make diagnosis more difficult. In order to reliably identify altered cells and tumours, this noise must be removed and both image quality and contrast enhanced.
Improving image quality achieves two important outcomes:
1. Improved diagnostic accuracy:
High-quality images allow radiologists to identify subtle tumours and distinguish malignant changes from benign ones – such as cysts or calcifications. Poor contrast or image noise can lead to false-negative or false-positive results. A false negative means a tumour is overlooked; a false positive may indicate a tumour that isn’t actually there – often leading to unnecessary biopsies.
2. More powerful AI models:
AI models are already supporting medical professionals in diagnostics. These models learn to recognise patterns from the image data they’re trained on. If trained with high-quality images, their performance improves significantly.
Noise and artefacts (image distortions) can mislead the model into learning incorrect patterns. Removing noise from an MRI scan allows the model to focus on actual anatomical structures instead of being distracted by random visual interference. So improving image quality benefits both humans and machines. There are two main ways to achieve this: through traditional methods (such as better hardware) and through deep learning – a subfield of artificial intelligence.
Traditional methods for enhancing medical images
Optimised hardware:
- In mammography, high-resolution detectors and compression techniques already help reduce tissue overlap and motion blur.
- Advanced MRI coil technology and stronger magnetic fields (e.g. 3 Tesla or 7 Tesla scanners) improve the signal-to-noise ratio (SNR). A high SNR means that the useful signal is much stronger than background noise, resulting in clearer, more detailed images.
Image processing techniques:
- Noise-reduction filters such as Gaussian or median filters reduce random noise in MRI images.
- Other techniques enhance contrast to make abnormalities more visible.
- Additional methods address motion artefacts caused by breathing or trembling – or artefacts resulting from metal implants.
While these traditional approaches are effective, they often require manual adjustments and are limited in handling complex noise patterns.
The solution: using deep learning to improve image quality
Salataris AI aims to support and enhance these traditional methods with deep-learning technologies. Deep learning involves artificial neural networks that analyse vast amounts of data to independently identify patterns and correlations. Unlike conventional software, these systems aren’t manually programmed but learn directly from the image data. With support from EuroCC Austria, the Salataris AI team trained several models – using both supervised and unsupervised learning – on the Italian supercomputer Leonardo. The goal: better images. All the techniques described here have already been successfully implemented.
Deep learning is particularly effective in detecting complex patterns in data, making it ideal for automated and optimised image enhancement. Salataris AI has used a variety of approaches:
Contrast-enhancing networks
It’s often difficult to differentiate tumours from healthy tissue in mammograms or MRI scans, especially when both appear similar in brightness. That’s where contrast-enhancing networks come in. These special deep learning models analyse the image and detect areas that may be diagnostically important – for example, suspicious structures or tissue changes. They then selectively adjust contrast in those areas, making tumour regions appear brighter or more defined, while surrounding healthy tissue is visually downplayed. The result is clearer images where potential tumours are easier to spot.
Generative Adversarial Networks (GANs)
GANs consist of two competing neural networks – one generates images, the other evaluates them. This “competition” leads to continually improved results, similar to an artist and a critic challenging one another. Salataris AI uses CycleGAN (Cycle-Consistent Generative Adversarial Network) to transform low-quality images into high-quality ones – for instance, sharpening blurry MRI scans. Another tool is SRGAN (Super-Resolution GAN), which enhances the resolution of low-quality mammograms without losing structural detail.
Unsupervised learning to remove artefacts
Unsupervised learning means that the deep learning model does not require predefined “correct” answers – no need for manually labelled images indicating which parts are tumours. Instead, the model identifies patterns by itself and learns to distinguish actual tumour features from noise or artefacts. This is done using convolutional neural networks (CNNs) such as U-Net, which can identify image regions likely to be artefacts and remove them – all without needing paired images (with and without artefacts) for training.
Denoising autoencoders
These neural networks compress noisy images into what’s called a latent space, then reconstruct a cleaner version. An encoder turns the image into a simplified representation (a kind of summary), and a decoder reconstructs an enhanced version of it. This reduces noise in both MRI and mammography images, while retaining important details like tumour boundaries.
The approach for training the AI: hyperparameter optimisation
During training, the aim was to test different models and continuously optimise their learning performance. This process is known as hyperparameter optimisation (HPO): developers search for the best possible configuration of the model and its training method. Since this involves a great deal of trial and error, significant computing power is required – which is exactly what a supercomputer provides. It allows many configurations to be tested in parallel, with the best-performing model selected at the end.
The team used several learning approaches at once, including:
- Unsupervised learning algorithms to remove image noise, enhance image quality and detect hidden features in rare or abnormal cases. Unsupervised learning means the model identifies patterns in the data without being told the correct answers – for example, whether dense tissue indicates a tumour.
- Supervised and semi-supervised learning: Supervised learning uses labelled data (e.g. “this image contains a tumour”) to train the model. Semi-supervised learning combines both labelled and unlabelled data.
- Manifold learning, which searches for hidden structures in complex datasets. A manifold is a mathematical structure that helps explain how complex, high-dimensional data may actually lie on a smooth surface – like a drawing on a crumpled sheet of paper: a two-dimensional surface distorted in space. In tumour detection, this means that MRI scans with similar features – like tumour boundaries – may lie close together on the same part of the manifold. The model tries to learn this structure to better identify changes in tissue.
- Contrastive learning, which helps the model distinguish clearly between similar and dissimilar cases.
- Self-adaptive learning, which allows the model to continuously adapt to new data and changing conditions. It keeps learning during operation and can use any learning type – supervised, semi-supervised, or unsupervised. This helps improve the model’s accuracy over time.
- Reinforcement learning via feedback: the AI system receives positive reinforcement for correct decisions and negative feedback for incorrect ones. This also improves its ability to recognise tumours – and to distinguish artefacts from true findings.
Free proof-of-concepts on European supercomputers
Deep learning bridges traditional diagnostics and the current demands of personalised, efficient medicine. When enhanced images are combined with tumour recognition algorithms, a positive feedback loop can emerge: better input data leads to more accurate models, enabling radiologists to make faster and more reliable decisions. Modern breast cancer diagnostics clearly benefit from optimised imaging. The foundation of these improvements is computing power – and Europe’s supercomputers are more than capable of handling the data load.
Through EuroCC, proof-of-concept access to supercomputing resources is free for start-ups and SMEs. For more information, please get in touch with our experts directly at: info@eurocc-austria.at.